Bio
Srinivasan (Srini) Venkatramanan is a research assistant professor at the Network Systems Science and Advanced Computing division. Prior to joining University of Virginia in 2018, Venkatramanan did his postdoctoral research at the Network Dynamics and Simulation Science Laboratory, Biocomplexity Institute of Virginia Tech (2015-2017), where he also worked as a Computational Health Data Scientist (2017-2018). He received his Ph.D. in Electrical Engineering from the Indian Institute of Science in 2014 for his dissertation titled "Influence Dynamics on Social Networks". Venkatramanan’s research areas include stochastic modeling, diffusion dynamics, optimal control and network science. At the Biocomplexity Institute, he is responsible for developing, analyzing and optimizing computational models for complex systems arising in the domains of epidemiology and food security.
-
Infectious disease modeling, model calibration and forecasting, Resource allocation optimization. Data synthesis, simulation analytics, network-based causal inference, and game theory
-
Indian Institute of Science, Bangalore, ECE, Ph.D., 2014
College of Engineering Guindy, Chennai, ECE, B.E., 2008
CausalGNN: Causal-based Graph Neural Networks for Spatio-Temporal Epidemic Forecasting
All models are useful: Bayesian ensembling for robust high resolution covid-19 forecasting
From 5Vs to 6Cs: Operationalizing Epidemic Data Management with COVID-19 Surveillance
A bridge-builder in the health district, a pair of professors who helped wrongfully convicted persons and a trio of scientists who analyzed the coronavirus early in the pandemic have been awarded this year’s University of Virginia public service awards.

A research team from the University of Virginia’s Biocomplexity Institute was recognized with the UVA Provost’s Office Award for Collaborative Excellence in Public Service. As representatives of the Biocomplexity Institute’s COVID-19 Response Team, Jiangzhuo Chen, Bryan Lewis, and Srini Venkatramanan were recognized for their service to the University, the Commonwealth of Virginia and federal authorities during the pandemic, and which continues today.
Srini Venkatramanan, research assistant professor at the Biocomplexity Institute, weighs in on the recent case numbers across California, Florida, and Texas.

Regarding the current COVID case data in the U.S., Srini Venkatramanan, Research Assistant Professor at the Biocomplexity Institute, told Newsweek that from the latest set of updates, short-term forecasts are pointed downwards, "hinting that we may have peaked as far as the Delta wave is concerned, at the national scale."

In this paper, researchers focus on a machine-learned anonymized mobility map aggregated over hundreds of millions of smartphones and evaluate its utility in forecasting epidemics, specifically the flu.

With increasing globalization, trade, and human movement, the rate of alien species introduction has increased all around the globe. This paper predicts the distribution of invasive species under conditions of climate change and is important for identifying susceptible areas of invasion and developing strategies for limiting their expansion.
On January 29, during a virtual ceremony over Zoom, the University of Virginia honored and recognized faculty members for their outstanding contributions to their fields and the impact of their research and scholarly activities at the annual Research Achievement Awards.

One of our research scientists, Srini Venkatramanan, was recognized as one of Intelligent Health’s top 50 innovators in 2020.

The UVA Biocomplexity Institute has received a $1.44M award from the National Science Foundation for a Virtual Organization (VO) that will facilitate communication and collaboration among CISE scientists currently involved in pandemic research through the NSF RAPID program.

As the COVID-19 pandemic continues to escalate in the United States and in many locations around the world, countless questions remain about next steps for mitigation and response. How will various mitigation methods affect the spread? How will those change as the pandemic progresses or regresses?
Researchers have developed a model that uses social-media and search data to forecast outbreaks of Covid-19 well before they occur.
Without enough test kits, the 1.3-billion-person country is using a gigantic surveillance network to trace and quarantine infected people.

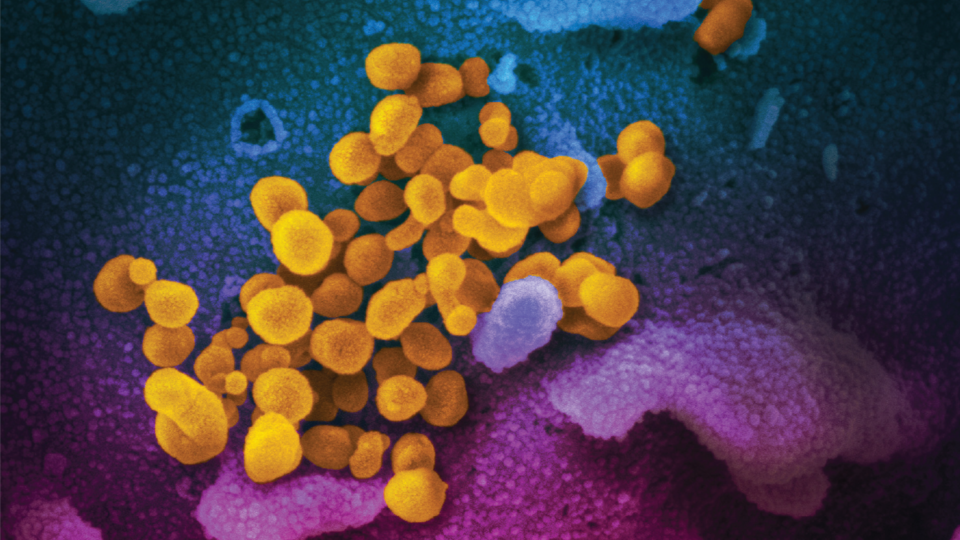
The 2019 Novel Coronavirus (COVID-19), which originated in Wuhan, China, in late 2019, has received significant global attention due to the rapid speed and widespread reach of the outbreak. As of early March 2020, COVID-19 has exceeded 92,000 confirmed cases in 76 countries within a span of two months. In response to this global pandemic, researchers from the University of Virginia’s Biocomplexity Institute have developed a series of visualization and analytical web applications to provide a greater understanding of the pandemic’s scope, and to help officials, healthcare systems, and policy makers worldwide, control and ultimately stop the outbreak.
Are influenza outbreaks and weather patterns connected? Researchers have long known that flu season occurs in the colder months, and that infection rates drop dramatically as the weather warms.

UVA researchers at the Biocomplexity Institute and Initiative are developing computational models to estimate and manage the biological, social and economic impacts of influenza.
While vaccination is the primary and most effective way to prevent sickness and death caused by flu, the CDC reports that less than 40 percent of Americans age 18 and older typically receive a flu shot. This begs the question: what additional mitigation and prevention methods might improve the public health response and policy development for the flu?